Community Paramedic Cuts Costs, Keeps People Out of Ambulances
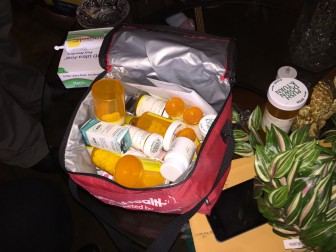
Community Paramedic Ben Thompson shows Delois Pearson, who suffers diabetes, how to handle syringes.
It’s been said that emergency responders’ jobs are 10 percent terror, 90 percent boredom. But there’s a new approach that lets them use their time more efficiently as they improve community health and even save money for cities and hospitals. It’s called “community paramedicine,” and it’s happening in Birmingham because of Fire and Rescue Service Lieutenant Ben Thompson.
Thompson tools around in his little white city-owned car. After teaching an elderly diabetic woman how to use and dispose of syringes and to avoid sugary sports drinks, Thompson thinks back to earlier trips to her North Birmingham neighborhood.
“When you’re on the fire engine, everybody knows, ‘oh yeah, that’s the Fire Department.’ But when you show up in this little car, people think, ‘what’s he doing, serving a warrant?’”
But soon, people begin to trust him and depend on him. And not just for themselves.
“The second time I come, they usually will stop me and say, ‘hey, will you come check on my aunt?’ I try to treat the neighborhood when I go see one person. It’s kind of like, you know, community policing? This is community paramedicine … just walking around the neighborhood, ‘hey, what do you need?’”
Thompson initially visits former hospital patients assessed as likely to be readmitted, and people who repeatedly call 911, including Mary Burke of Ensley. She suffers high blood pressure, diabetes, and nerve issues. She used to call ambulances all the time.
“Until I met him,” she interjects with a laugh. Thompson helps her arrange doctor’s appointments and helps her manage her medications. She’s supposed to take heart medicine twice a day.
“She was taking it twice a day,” he points out. “However, she was taking it at eight in the morning, and then around lunch. So, she was having problems with feeling kind of weak and feeling like her heart was beating really hard, so I said, ‘hey, maybe you’re taking your beta-blocker a little too close together,’ so … now she’s changed [her regimen].”
Taking the second dose later in the day made all the difference.
“I feel much better,” says Burke. “I can accept getting up, and doing about like I used to. And I thank God for him.”
Often it’s just that kind of basic information that keeps Mary Burke and a few dozen others out of emergency rooms. That lightens the load on caregivers, too, including Mary’s son Toby Burke. He cooks and cares for both his parents.
Thompson’s visits “take a lot of stress off me, and I can hang up my doctor’s license,” he says with a clearly inherited laugh. He likes the idea of taking stress off emergency responders, too.
“Now, thankfully and hopefully, we won’t have to call 911, so that way they can fight fires and, you know, help other people.”
That’s already happening. Assistant Fire Chief Donald Jones says Thompson has reduced preventable 911 calls, which saves the city money and saves responders for other calls.
“It actually makes it a lot safer for everybody,” says Jones. “Us and the citizens. It’s a win-win for everybody.”
Hospitals win too. Dr. Anne-Laura Cook, a community health specialist, coordinates a partnership between Thompson and Princeton Baptist Medical Center; hospital staff give Thompson lists of patients assessed as high-risk for being readmitted.
“A lot of insurance companies, particularly Medicare, are now penalizing hospitals for patients that return to the hospital within 30 days,” she says. “The Birmingham Fire and Rescue community paramedicine service can intervene, so it results in fewer emergency department visits.”
And it’s good business for the hospital for another reason.
“We’re hopeful that if someone is sick … and does feel the need to come to a hospital facility, because of our program and our collaboration in the community, and our ability to get things done in a nontraditional way, they would choose to come to us.”
So building those relationships has benefits. It has drawbacks, too, especially for Thompson.
“When you’re at the fire station and you just respond on a call and [the victims] have passed away, that’s one time you see them – one call of ten a day. But me, I’ve gotten to know these people, so when they pass away … that’s a life I knew in my life that’s gone … their story is over … it’s heavy.”
Even so, Thompson says the upside of that emotional coin outshines the downside.
“With this [paramedicine approach], we actually get to go see them every day … I know what’s happening with them, so it’s very rewarding. I suggest any paramedic who’s been doing it for a long time, maybe feeling a little burned out: try this. It’ll make you feel a lot better about what you do.”
Thompson is beginning to collect data on the program’s effectiveness. That could be useful when he starts looking for grants to expand it beyond himself and the occasional colleague, nursing student, or social-work student who rides along.
At the end of our ride-along, a radio call about an unconscious woman comes in. Even in a car with no sirens or flashers, Thompson arrives first. That’s because he was already out there … in the neighborhood.
The woman wasn’t breathing, but Thompson helped revive her.
With temporary protections for some Afghans set to expire, appeals court steps in
An appeals court late Monday stepped in to keep in place protections for nearly 12,000 Afghans that have allowed them to work in the U.S. and be protected from deportation.
HBO’s new Billy Joel documentary is revelatory — even if it pulls some punches
The new two-part documentary, which premieres Friday on HBO, is a good example of the tension between access and objectivity that filmmakers face in making documentaries on celebrities.
A wildfire destroyed the historic Grand Canyon Lodge. It burned down once before
The Grand Canyon Lodge is the only hotel on the park's North Rim, which is closed for the rest of the season due to wildfire risk. The hotel was already rebuilt once, after a kitchen fire in 1932.
Why the Federal Reserve’s building renovations are attracting the White House’s ire
The Fed's $2.5 billion headquarters renovation is attracting mounting criticism from the Trump administration, which had been already attacking the central bank for not cutting interest rates.
Supreme Court says Trump’s efforts to close the Education Department can continue
The Trump administration had appealed a decision that had directed it to stop gutting the U.S. Education Department and to reinstate many of the workers the government had laid off.
Trump tells supporters not to ‘waste time’ on Epstein files. They’re not happy
President Trump is facing backlash from his supporters and opponents alike for how his administration has handled the release of evidence surrounding the death of disgraced financier Jeffrey Epstein.